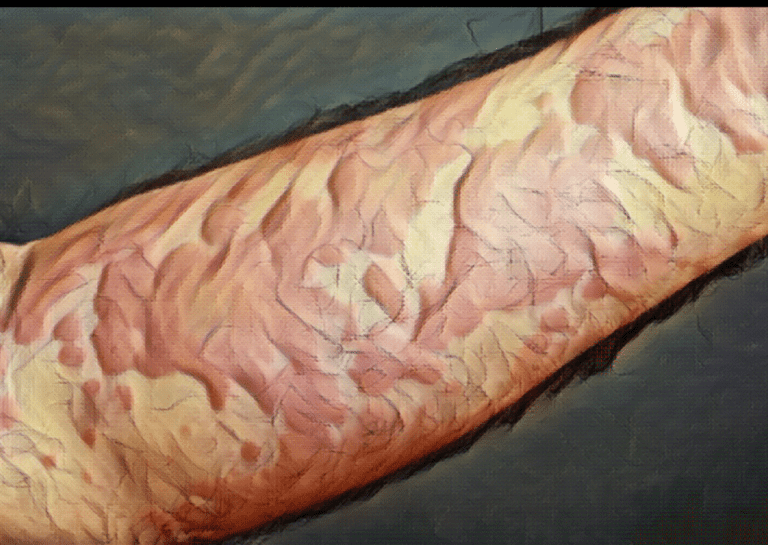
Overview
Babies and children are susceptible to allergic reactions from a number of different sources, such as food, bath soaps, laundry detergents, or medication. An allergic reaction occurs when the body or the immune system responds negatively to certain substances that would otherwise have no side effects.
Because of their sensitive skin and delicate digestive systems, babies are especially prone to having adverse reactions to food and other common substances. While skin allergies often persist into adulthood, certain food allergies resolve themselves in childhood or adolescence.
Common types of allergies
Skin allergies
Skin allergies typically consist of a delayed inflammatory response to contact allergens that can be found in everyday substances such as creams, soaps, food, perfumes, and cosmetics.
- Eczema — This is an inflammatory skin disease that can be caused by contact allergy to topical creams or medications. Symptoms include a red, itchy rash, hot or inflamed skin, cracks in skin, bleeding/oozing, and difficulty sleeping. Eczema can be caused by soaps, detergents, and topical emollients. The condition may also be exacerbated by environmental conditions such as cold and dry weather, or food allergies.
- Allergic contact dermatitis — This is an acquired condition characterized by inflammation of the dermis and epidermis. The allergic reaction occurs when the skin comes into contact with an allergen, but the inflammatory response can be delayed by several days. Allergens include food and cosmetic additives such as nickel, cobalt, and carmine; emollients such as lanolin (used to treat diaper rash and skin irritation); and fragrances. Common symptoms are redness, itching, and dry, flaky skin that may ooze or burn [4].
Food Allergies
Food allergies generally appear in babies before their second birthday and typically peak at one year of age. Some food allergies, such as those involving cow’s milk and hen’s eggs, will usually be outgrown before adolescence or adulthood.
- Milk allergy — Cow’s milk allergy (CMA) is the most common type of food allergy in babies and children. The majority of children with CMA will have an allergy to another food too. CMA involves an adverse reaction to the proteins found in milk, and generally occurs once milk is introduced into the baby’s diet through cow’s-milk-based formula, solid foods containing cow’s milk proteins, or in rarer cases, through the mother’s breast milk. Symptoms include skin conditions such as eczema or dermatitis, red bumps or hives, facial swelling, colic, persistent cough, vomiting, and diarrhea.
- Hen’s egg allergy — Another common type of food allergy, hen’s egg allergy, affects up to 9 percent of children [3]. The allergic reaction occurs as a result of an adverse immune response to the proteins in domestic chicken eggs. The severity of the reaction can sometimes depend on the form of egg consumed, e.g. egg white or egg yolk, raw or cooked egg. In a 2 year study, researchers found egg allergy resolved in 47% of infants, by 2 years of age. However, resolution was lower in children with baked egg allergy at age 1 year (13%) compared with baked egg tolerance (56%). Symptoms of hen’s egg allergy usually manifest in the skin, but there may also be gastrointestinal or respiratory symptoms. These symptoms include itching, hives, inflammation, vomiting, stomach cramps, coughing, shortness of breath, and congestion.
- Peanut and tree nut allergy — Peanut and tree nut allergies affect around 3 percent of children, with 20 to 25 percent developing a tolerance to the allergens over time. The two types of nut allergy are not the same, however. A tolerance for peanuts does not automatically indicate a tolerance for tree nuts too. Allergic reactions often involve the skin, gastrointestinal tract, and respiratory tract. Symptoms include hives, swelling around the mouth, tightening in the throat, stomach cramps, and vomiting.
Diagnosis
Allergic reactions can be divided into two types depending on whether they are or are not triggered by an antibody called Immunoglobulin-E (IgE) — IgE-mediated and non-IgE-mediated. The symptoms for each type of reaction can vary.
- IgE-mediated allergies are the most common type and involve a reaction of the IgE antibody. Reactions usually occur shortly after consumption or exposure to the responsible allergen.
- Non-IgE-mediated allergies involve a component of the immune system other than IgE, and reactions of this type are often delayed.
If you suspect your child has an allergy, you should seek a referral from your pediatrician or doctor to have them seen by an allergy specialist. Allergy testing should be carried out by a specialist trained in handling allergic reactions and anaphylaxis.
Skin testing is the fastest and most cost-effective way to diagnose IgE-mediated allergies, with the prick/puncture technique and the intradermal technique being the most common methods. Results are often ready within 20 minutes of testing, giving parents immediate clarity on their children’s potential allergies.
Management
Allergy management involves avoiding the specific allergens that trigger allergic reactions. Depending on the severity of the allergy, substances such as certain foods, skincare products, and cosmetics may need to be avoided or eliminated entirely from the child’s environment to prevent future reactions.
Skin allergies may need to be managed using medicated topical creams. Consult your pediatrician or dermatologist for advice on creams and medications. Peanut allergy sufferers may be advised to carry an epinephrine auto-injector — commonly known as an EpiPen — to treat anaphylaxis caused by accidental consumption or contact with peanuts.
References
- Peters RL, Allen KJ, Dharmage SC, et al. Natural history of peanut allergy and predictors of resolution in the first 4 years of life: A population-based assessment. J Allergy Clin Immunol 2015; 135:1257.
- Peters RL, Koplin JJ, Gurrin LC, et al. The prevalence of food allergy and other allergic diseases in early childhood in a population-based study: HealthNuts age 4-year follow-up. J Allergy Clin Immunol 2017; 140:145.
- Peters RL, Dharmage SC, Gurrin LC, et al. The natural history and clinical predictors of egg allergy in the first 2 years of life: a prospective, population-based cohort study. J Allergy Clin Immunol 2014; 133:485.
- Ruëff F, Bergmann KC, Brockow K, et al. [Skin tests for diagnostics of allergic immediate-type reactions. Guideline of the German Society for Allergology and Clinical Immunology]. Pneumologie 2011; 65:484.
- Stiefel G, Anagnostou K, Boyle RJ, Brathwaite N, Ewan P, Fox AT, Huber P, Luyt D, Till SJ, Venter C, Clark AT. BSACI guideline for the diagnosis and management of peanut and tree nut allergy. Clin Exp Allergy. 2017 Jun;47(6):719-739. doi: 10.1111/cea.12957. PMID: 28836701.