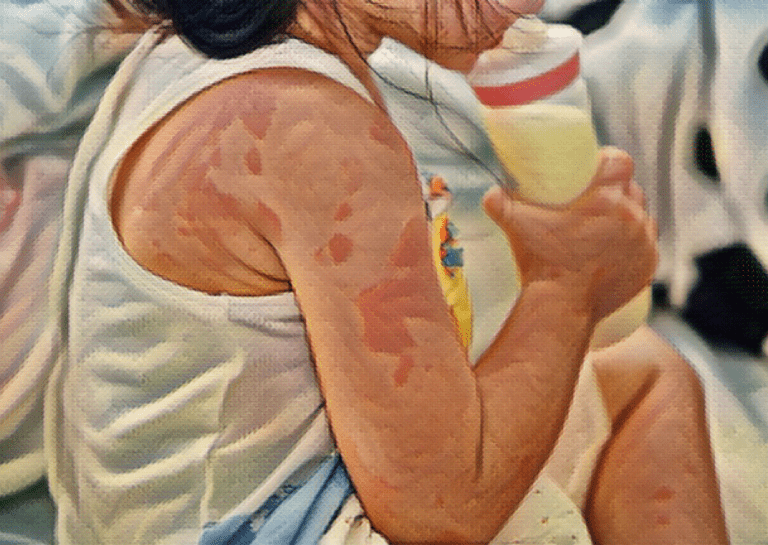Milk allergies are some of the most common food allergies seen in babies and young children. These allergies arise from an adverse reaction to the proteins found in the milk of cows and goats.
Cow’s milk allergy is the most prevalent form, affecting around 2 percent of infants under the age of 4. Cow’s milk allergy primarily affects children, as most adults will have developed a tolerance to milk proteins by the age of sixteen, if not younger.
Table of contents
Development
Cow’s milk allergy can develop in babies when milk is introduced into their diet through cow’s-milk-based formula, or, in rarer cases, through their mother’s breastmilk. Symptoms can appear within days or weeks of consumption. For some babies, the reaction will occur immediately after consuming milk and may affect the skin, throat, and respiratory tract.
Symptoms
Allergic reactions to cow’s milk can vary widely, with symptoms ranging from mild to life-threatening. Cow’s milk allergy can be confused with other conditions that cause similar symptoms, such as colic, GERD (reflux), and constipation.
Symptoms commonly associated with cow’s milk allergy include:
- Itchy rashes
- Eczema
- Facial swelling
- Colic
- Vomiting
- Feeding difficulties
- Weight loss
- Cough
- Congestion
- Fever
- Constipation
- Diarrhea
If you suspect that your baby is having adverse reactions to cow’s milk, you should see a pediatrician. You should also seek medical advice if your baby displays a combination of the above symptoms or develops a fever (100.4˚F or higher).
Diagnosis
Like other common food allergies, cow’s milk allergy can be difficult to diagnose because the symptoms are not exclusive to this condition. Milk allergies should be tested by an allergy specialist who is trained in handling serious allergic reactions.
The most accurate procedure for diagnosing milk allergy is a clinician-supervised oral food challenge. Other tests for diagnosing milk allergy are skin prick tests and lab tests for the presence of antibodies produced by allergic reactions to milk.
If these tests are inconclusive, an allergy specialist may recommend that you eliminate milk from your baby’s diet for a period of 2 to 8 weeks. For breastfed infants, this means that the mother must also eliminate milk from their diet. If your baby is formula-fed, you will be required to switch to a non-milk-based formula for this period.
Management
Most babies who develop a milk allergy will build up a tolerance by the age of 3. But if your baby is diagnosed with a milk allergy, you will need to manage the allergy to avoid future reactions.
Proper allergy management involves changing your baby’s diet to avoid cow’s milk and replacing it with an alternative source of protein and calcium. It is also important to ensure all possible caretakers are made aware of the baby’s new dietary requirements.
Breastfeeding mothers may need to manage their own milk-protein consumption to avoid transmitting allergens to the infant.
Avoiding milk proteins in your baby’s diet can be difficult. Finding an appropriate replacement is essential for their nutritional health and wellbeing though. An amino-acid or soy-based formula can be used as an alternative to cow’s milk-based formula.
Always consult an allergy specialist or pediatrician when learning how to manage a food allergy and before making changes to your baby’s diet.
References
Heine RG, Elsayed S, Hosking CS, Hill DJ. Cow’s milk allergy in infancy. Curr Opin Allergy Clin Immunol. 2002 Jun;2(3):217-25. doi: 10.1097/00130832-200206000-00011. PMID: 12045418.
Høst A. Cow’s milk protein allergy and intolerance in infancy. Some clinical, epidemiological and immunological aspects. Pediatr Allergy Immunol. 1994;5(5 Suppl):1-36. PMID: 7704117.
Luyt D, Ball H, Makwana N, Green MR, Bravin K, Nasser SM, Clark AT; Standards of Care Committee (SOCC) of the British Society for Allergy and Clinical Immunology (BSACI). BSACI guideline for the diagnosis and management of cow’s milk allergy. Clin Exp Allergy. 2014;44(5):642-72. doi: 10.1111/cea.12302. PMID: 24588904.
Skripak JM, Matsui EC, Mudd K, Wood RA. The natural history of IgE-mediated cow’s milk allergy. J Allergy Clin Immunol. 2007 Nov;120(5):1172-7. doi: 10.1016/j.jaci.2007.08.023. Epub 2007 Nov 1. PMID: 17935766.